A Guide to Healthcare System Integration Services
At its heart, healthcare system integration is about connecting the dots. Think of all the different software and applications your organization uses: the Electronic Health Record (EHR), the lab information system, the pharmacy, billing, and radiology. Integration services are the specialized processes and technologies that get these separate systems talking to each other.
The whole point is to create a single, unified network where critical data flows freely. When a patient’s records, lab results, and billing information are all in sync, clinicians get what they’ve always needed: a complete, real-time view of the patient.
Why Connected Healthcare Is No Longer Optional
Let's paint a quick picture. A patient rushes into the emergency room. Their family doctor has their medical history, a cardiologist has recent EKG results, and their local pharmacy has a full list of their medications. Without integration, these are just scattered puzzle pieces. The ER doctor is left trying to make life-or-death decisions with only a fraction of the story.
This isn't a hypothetical; it's a daily reality that leads to redundant tests, dangerous medication errors, and delays in critical care. Healthcare system integration services essentially act as the central nervous system for a modern healthcare organization. They bridge the gaps between all these disparate software systems, making sure a patient's complete, up-to-date story is available to any authorized provider who needs it. This isn't just a tech upgrade; it’s a fundamental change in how medicine is practiced.
Before we go deeper, it helps to see a side-by-side comparison of just how stark the difference is between a disconnected and an integrated environment.
Comparing Disconnected vs. Integrated Healthcare Systems
This table breaks down the real-world impact of system integration on core healthcare functions, highlighting the shift from inefficiency and risk to safety and streamlined operations.
| Area of Impact | Disconnected Systems (The Problem) | Integrated Systems (The Solution) |
|---|---|---|
| Patient Care | Fragmented patient history leads to potential misdiagnoses, duplicate tests, and adverse drug events. | Clinicians have a complete, 360-degree patient view, enabling safer, more informed decisions at the point of care. |
| Clinical Workflow | Staff waste hours manually entering data, making calls to track down records, and toggling between multiple systems. | Automated data flow reduces manual work, freeing up clinicians to spend more time with patients. |
| Patient Experience | Patients are frustrated by repeating medical histories and undergoing unnecessary procedures. | A seamless experience where a patient’s information follows them across departments and facilities. |
| Operational Efficiency | Billing errors, scheduling conflicts, and revenue cycle delays are common due to mismatched data. | Accurate, real-time data exchange streamlines administrative tasks, reduces claim denials, and improves financial health. |
| Data & Analytics | Meaningful population health analysis is nearly impossible when data is trapped in isolated systems. | A unified data source allows for powerful analytics, identifying trends for better public health and operational planning. |
As you can see, the move toward integration addresses some of the most persistent and costly challenges in the industry. It’s about building a system that works for people – both the patients and the providers who care for them.
The Problem of Data Silos
The core issue that integration solves is the data silo. When vital patient information is locked away in one department’s software, it creates a domino effect of problems that hurt patient outcomes and your bottom line.
-
Clinical Inefficiencies: Doctors and nurses spend far too much time playing detective: chasing down lab results, calling other departments for records, and manually re-entering data that already exists somewhere else.
-
Increased Risk of Errors: An incomplete patient history is a recipe for disaster. It dramatically raises the risk of medication conflicts, missed allergies, and other preventable medical errors.
-
A Poor Patient Experience: Nothing frustrates patients more than having to repeat their entire medical story at every single appointment or undergoing the same test twice because the results weren’t shared.
-
Operational Bottlenecks: On the administrative side, disconnected systems are a nightmare for billing, scheduling, and managing the revenue cycle, leading to constant delays and lost income.
The Shift to Interoperability
Thankfully, the industry is moving decisively to fix this. With the widespread adoption of EHRs and government mandates pushing for digital health, the demand for seamless data exchange has never been higher. In fact, the global Healthcare IT Integration Market is expected to grow at a strong 11.52% CAGR from 2026 to 2033, a clear sign that organizations are investing heavily in connectivity. You can get more details on this market trend in the full report.
Interoperability is the ultimate goal here. It’s more than just connecting systems; it’s the ability for those different systems to communicate, exchange data, and actually use the information that has been shared. Without it, the true promise of digital health simply can’t be realized.
Achieving this level of sophisticated connectivity takes a partner with deep expertise in both healthcare workflows and complex technology. For a dedicated healthtech software development partner, the primary mission is to engineer the exact solutions that break down these silos for good. By building a truly unified data ecosystem, your organization can finally leave the fragmented past behind and become more patient-centric, efficient, and data-driven.
Understanding the Building Blocks of Integration
For any healthcare system to talk to another, they need two basic things: a shared language and a reliable way to pass messages back and forth. Think of it like organizing a global conference. You need translators so everyone understands each other, and you need a solid communication network to connect the speakers with the audience. The technologies that make healthcare integration possible work in much the same way, creating the structure for data to flow where it’s needed.
This need for connected care is driving significant market growth. The Healthcare and Medical System Integrators Market was valued at USD 2,342 million in 2025 and is on track to hit USD 5,750 million by 2033, growing at a strong 11.88% CAGR. This surge is a direct response to the push for digital healthcare and the overwhelming demand for unified, patient-focused systems. You can get a deeper dive into the market forecast and its drivers here.
This diagram perfectly illustrates the difference between a disconnected system, where data gets trapped in silos, and a fully integrated one where information flows freely.
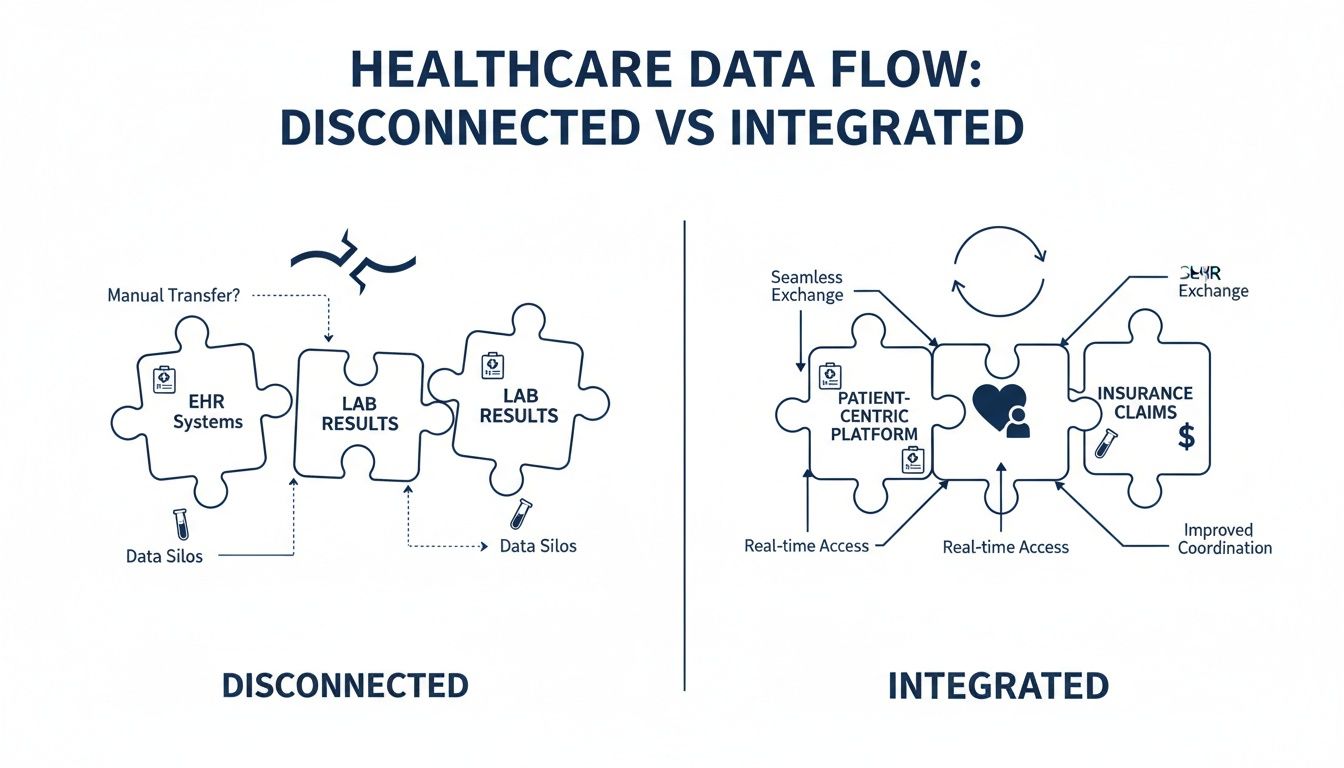
As you can see, integration isn’t just about connecting software; it’s about turning fragmented data points into a complete patient story. That’s the real foundation of modern care delivery.
The Languages of Healthcare Data: HL7 and FHIR
At the very core of integration are data standards. These are the grammar and vocabulary that allow different systems to understand health information. Two standards really run the show:
-
HL7 (Health Level Seven): This is the old guard, the established workhorse of healthcare data. Think of it as the formal, highly structured language used in official documents. HL7 is exceptionally good at packaging clinical information, like admissions, lab orders, and test results, into a predictable format. It’s been the reliable standard for communication between big systems like EHRs and lab information systems for decades.
-
FHIR (Fast Healthcare Interoperability Resources): This is the new kid on the block, built for the modern, internet-driven world. If HL7 is formal grammar, FHIR is more like a flexible, conversational dialect designed for the web. It uses the same kind of modern standards that power today’s websites and apps (like RESTful APIs), making it much easier to share data with mobile devices, patient portals, and cloud-based tools. This flexibility greatly simplifies the work of custom healthcare software development.
While HL7 is still critical for a lot of internal, system-to-system communication, FHIR is quickly becoming the go-to standard for any scenario that involves sharing data with patients or external applications.
APIs: The Digital Messengers
If HL7 and FHIR are the languages, then Application Programming Interfaces (APIs) are the messengers carrying the conversations. An API is simply a set of rules that lets one piece of software talk to another to request data or services.
Here’s a simple analogy: think about ordering from a restaurant. You don’t go into the kitchen yourself. Instead, you give your order to a waiter (the API), who takes it to the kitchen (the other system) and brings your food (the data) back to you. In a hospital, an API might carry a request from a doctor’s smartphone app to the main EHR to pull up a patient’s latest lab results. This controlled give-and-take is central to all modern custom software development.
Middleware: The Central Hub
In a busy hospital with dozens of different systems, trying to connect each one directly to every other one would be pure chaos. This is where middleware, often called an integration engine, saves the day.
An integration engine works like an airport’s air traffic control tower. Instead of every system creating a separate connection to every other system, they all just connect to the central hub. This engine handles all the heavy lifting: translating messages between different formats (like from HL7 to FHIR), routing them to the right destination, and making sure everything is delivered securely.
EHR Connectors: The Pre-Built Adapters
Finally, we have EHR connectors. These are essentially pre-built adapters made specifically for major EHR platforms like Epic, Cerner, or Allscripts. Building a brand-new interface from scratch for each EHR is incredibly time-consuming and expensive.
Connectors are like having a universal travel adapter for your electronics; they provide a standardized, ready-to-go link that dramatically speeds up the integration process. Using them is a smart strategy often found in advanced product engineering services.
The Tangible Business Case for Integration
Alright, the tech is impressive, and having data flow seamlessly sounds great. But for any executive or decision-maker, it all comes down to one question: what’s the actual return on this investment?
A smart integration plan pays for itself in several concrete ways. It’s not just about theory; we’re talking about measurable gains that directly boost your bottom line and improve patient care. These initiatives often fall under the umbrella of expert digital transformation consulting, which is really about connecting the tech solutions to your most important business goals. When you get this right, you stop just putting out fires and start making proactive, data-informed decisions.
Slashing Operational and Clinical Costs
One of the first places you’ll see a financial win is in cutting down operational waste. Disconnected systems create a constant drain on resources because they force your staff into manual workarounds and redundant processes.
Integration goes straight to the source of these inefficiencies:
-
Eliminating Duplicate Tests: Imagine a clinician can instantly see a patient’s full history, including recent labs and scans from another department. The need for repeat tests disappears. You’re not just saving money on the test itself, but also on all the labor and materials that go with it.
-
Automating Administrative Tasks: Think about the hours your team spends on the phone verifying patient info, punching the same data into three different systems, or hunting for a missing file. Integrated systems handle that data flow automatically. This frees up your skilled staff to focus on what truly matters: patient care. One study found that moving to a more integrated, cloud-based infrastructure led to a 70% drop in critical incidents and saved clinicians a collective 144,000 hours.
This is exactly the kind of efficiency that modern custom healthcare software development aims to deliver. It’s about getting rid of the operational drag so you can run a much leaner, more effective organization.
Improving Clinical Outcomes and Patient Safety
A unified patient view isn’t just a nice-to-have; it’s a critical tool for boosting patient safety and achieving better clinical results. And better outcomes have a direct financial upside by cutting down on costly complications, readmissions, and penalties. Giving a clinician the complete picture at the point of care empowers them to make the best possible decision, every time.
A study from the University of Michigan revealed something staggering: a lack of information sharing between providers contributes to nearly $76 billion in medical errors each year. Integration is the most direct solution to closing this dangerous and expensive information gap.
Connected systems act like a digital safety net. For instance, when your EHR can talk to your pharmacy system, it can automatically flag a potential drug interaction or allergy before a prescription is even filled. Fewer medical errors mean lower malpractice liability and help you avoid the steep government penalties tied to poor safety scores.
On top of that, a complete patient record allows for much better management of chronic diseases. This, in turn, leads to fewer hospital readmissions – a key performance metric that is now directly tied to financial reimbursements.
Using AI and Automation in Integrated Systems
Think of integration as building the superhighway for your organization’s data. But a highway is just asphalt without cars and a smart traffic control system. This is where artificial intelligence and automation come in; they provide the intelligence that directs the flow of information, turning a passive data pipeline into a living, breathing asset that actively works for you. This process is a key part of our AI transformation framework, which guides organizations in leveraging AI effectively.
This shift couldn’t be happening at a better time. The Healthcare IT Market is on track to grow by a staggering USD 247.22 billion between 2026 and 2030, largely because hospitals are finally getting serious about using AI, IoT, and big data to improve patient care and slash readmission rates. We’re seeing this firsthand as advanced AI is embedded directly into EHRs, signaling a fundamental move toward smarter healthcare. For a closer look at this market expansion, Grand View Research offers a detailed analysis.

The goal is no longer just to connect systems that store data; it’s to build systems that use it. By working with seasoned AI development services, healthcare leaders can discover what it truly means to implement AI for your business and evolve from basic connectivity to intelligent, decisive action.
From Reactive to Predictive Analytics
A fully integrated system is the perfect launchpad for predictive analytics. Instead of just reacting to problems after they’ve already happened, you can start anticipating them. Machine learning models thrive on these kinds of unified datasets, analyzing vast amounts of information to spot subtle patterns a human could never see.
This unlocks some truly powerful capabilities:
-
Forecasting Patient Risks: AI can analyze a patient’s complete history: labs, vitals, genomics, and more, to calculate their risk of developing sepsis or suffering a post-op complication. This gives your clinical team a priceless head start to intervene before a crisis occurs.
-
Predicting Operational Bottlenecks: By looking at appointment schedules, staffing levels, and real-time patient flow, machine learning can predict an ER rush or a slowdown in the OR. This gives managers the chance to reallocate staff and resources before a bottleneck forms.
-
Anticipating Disease Outbreaks: On a community level, aggregated and anonymized data from multiple facilities can reveal the early whispers of a flu outbreak or other public health trends, giving everyone time to prepare.
Unlocking Unstructured Data with NLP
So much of a patient’s real story is buried in unstructured text: the detailed, narrative notes from clinicians, radiologists, and specialists. This information is a goldmine of context, but it has always been incredibly difficult to analyze in any systematic way.
This is where Natural Language Processing (NLP), a specialized field of AI, comes into its own. NLP gives computers the ability to read and make sense of human language, pulling critical facts out of those dense clinical notes.
Picture an NLP-driven tool that constantly scans physician notes to:
-
Identify undocumented patient allergies or a family history of disease.
-
Flag a discrepancy between a doctor’s narrative and the formal diagnosis code.
-
Pull out key symptoms described in the patient’s own words to help build a more accurate diagnosis.
Suddenly, a static block of text becomes a searchable, actionable source of life-saving intelligence.
Automating High-Volume Workflows
Finally, AI-powered automation is your best weapon against the repetitive, soul-crushing tasks that lead to staff burnout. Layering AI on top of an integrated system allows you to intelligently automate workflows that used to need constant human intervention. As we explored in our guide to clinical workflow automation solutions, these tools are a total game-changer.
Just consider a few examples:
-
Intelligent Routing: An AI can instantly route critical lab results from the lab system directly to the on-call specialist’s secure mobile app, cutting out delays and middlemen.
-
Automated Prioritization: AI can scan incoming radiology reports, identify abnormal findings, and automatically push them to the top of the radiologist’s reading list.
-
Administrative Automation: Tasks like sending appointment reminders, verifying insurance eligibility, and suggesting billing codes can be automated with near-perfect accuracy, freeing your administrative team to focus on patients, not paperwork.
By adding this layer of intelligence, healthcare system integration moves beyond simply connecting data. It creates a smarter, more efficient, and fundamentally safer environment for everyone.
Navigating Security and Compliance Challenges
Every time you connect another system, you’re essentially adding a new door to your digital house. While healthcare system integration services are designed to open up communication between your tools, they also expand your digital footprint. This creates more potential entry points for security threats, making robust security and compliance an absolute necessity, not just an afterthought.
This isn’t just about good IT practice; it’s about the law. Strict regulations like the Health Insurance Portability and Accountability Act (HIPAA) in the U.S. and the General Data Protection Regulation (GDPR) in Europe dictate exactly how Protected Health Information (PHI) must be handled. A single mistake can lead to devastating fines, legal battles, and a loss of patient trust that can take years to rebuild.

Core Security Measures for Integrated Systems
To properly defend this newly interconnected environment, a few security controls are non-negotiable. Think of them as layers of armor that work together to shield sensitive data at every step.
-
End-to-End Encryption: Data must be scrambled and unreadable, whether it’s sitting idle in a database (at rest) or being passed between applications (in transit). If a bad actor gets their hands on it, it’s completely useless to them.
-
Role-Based Access Control (RBAC): Not everyone in the hospital needs to see every patient’s full history. RBAC enforces the principle of least privilege, ensuring people can only see and do what is absolutely necessary for their specific job.
-
Comprehensive Audit Trails: Every time someone accesses, changes, or shares patient data, it needs to be logged. These detailed records are your first line of defense for spotting suspicious activity and are crucial for proving compliance during an audit.
These same secure technologies can also boost efficiency. For example, AI-driven tools like virtual medical receptionist services can handle routine patient calls and appointments, freeing up your staff while operating within these strict, secure access rules.
Proactive Defense and Partnering for Compliance
Waiting for an attack to happen is a losing game. A modern security strategy has to be proactive, constantly searching for weaknesses before someone else does. This means bringing in independent experts for regular security audits and penetration testing, where ethical hackers try to break into your systems to find the cracks. As we explored in our guide, building security in from day one is a core tenet of any HIPAA-compliant application development.
The complexity of modern healthcare security means that going it alone is a significant risk. Building a secure, integrated system requires specialized expertise that few in-house IT teams possess.
This is precisely why choosing the right partner is so important. You need a team that offers dedicated cyber compliance solutions. A great partner doesn’t just connect your systems; they architect the integration with security built into its very foundation. They live and breathe healthcare regulations and know how to build a network where data is both instantly available to authorized clinicians and ironclad against ever-present threats.
How to Choose the Right Integration Partner
Let’s be blunt: choosing your integration partner is the single most important decision you’ll make in this entire process. Get it right, and you have a strategic guide who helps you navigate the complexities of healthcare tech. Get it wrong, and you’re looking at budget blowouts, compliance nightmares, and a project that’s dead on arrival.
A great partner doesn’t just ask for a spec sheet and start coding. They dig in, ask the tough questions, and bring a deep understanding of clinical workflows to the table. They should function as a consultant first, helping you map out a phased implementation that delivers clear wins at every step.
The Vendor Selection Checklist
When you’re vetting potential partners, you need to cut through the sales pitch. A solid firm will have confident, detailed answers to these questions.
-
Proven Healthcare Experience: Have they actually done this before? Ask to see their portfolio of client cases. You’re not just looking for pretty websites; you’re looking for proof that they understand the unique pressures and workflows of a healthcare environment.
-
Technical Proficiency in Standards: How fluent are they in HL7 and FHIR? Do they have real-world API development experience in a clinical setting? They must be experts in the languages that make healthcare data move.
-
Scalability and Future-Proofing: Will the system they build today still work in five years? Their proposed architecture needs to be flexible, ready to handle more data and new technologies without a complete teardown.
-
A Consultative, Strategic Approach: Do they want to understand your business goals, or do they just want to talk about technology? A true partner helps you build a strategy, not just a product.
Of course, none of this matters if security isn’t baked in from day one. A practical guide to HIPAA compliance for handling patient data isn’t just recommended reading; it’s the law. Your partner has to prove they can build a fortress around patient data, not just an integration.
Vendor vs. Dedicated Team
It’s also crucial to think about the working relationship. Are you hiring a vendor for a one-time project, or are you bringing on a dedicated development team that will feel like a long-term part of your own organization?
A vendor completes a task. A dedicated team invests in your success. For a complex, ongoing initiative like system integration, the dedicated team model offers superior alignment, deeper institutional knowledge, and greater flexibility as your needs evolve.
This model creates a partnership where the external team is fully bought into your culture and long-term vision. As we’ve covered in our guide to choosing a medical systems integration partner, that alignment is the secret ingredient for navigating complex, multi-year projects.
The Importance of Ongoing Support
Finally, remember that integration isn’t a one-and-done project. It’s a journey. Your systems will evolve, regulations will change, and your business needs will shift. The best partners know this and plan for it, offering robust support and maintenance to keep your integrated ecosystem secure, efficient, and compliant.
They become your long-term healthtech software development partner, there to help you adapt and grow. At the end of the day, you aren’t just picking a vendor – you’re choosing a relationship. Make sure it’s one built to last.
Your Healthcare Integration Questions Answered
If you’re exploring healthcare system integration services, you probably have a lot of questions. We get it. Here are some of the most common ones we hear from healthcare leaders, along with clear, practical answers from our experience in the field.
What is the difference between integration and interoperability?
This is a great starting point, and the distinction is crucial. Think of it this way: Integration is the physical work of building the tracks and connecting two separate train stations. You’ve established a pathway.
Interoperability, on the other hand, is what happens after the tracks are laid. It’s the ability for trains from both stations to run on those tracks, understand the signals, and seamlessly exchange passengers and cargo. In healthcare, integration is the technical “how,” but true interoperability is the goal – making sure connected systems can actually exchange and use data in a meaningful way to improve care.
How long does a typical healthcare integration project take?
The timeline really depends on the complexity of the project. We’ve seen simple, point-to-point connections take just a few weeks, especially when connecting two modern systems using standard FHIR APIs (like linking a new lab information system to an EHR).
However, a more ambitious project, say, one that involves multiple legacy systems, a central integration engine, and custom software development, can easily take six to twelve months, or even longer. The scope of the project, the quality of your existing data, and the availability of modern APIs are the biggest factors influencing the timeline. That’s why we almost always recommend a phased approach to show value early and often.
What are the biggest challenges in healthcare integration?
In our experience, teams almost always hit one of three major roadblocks:
-
Data Standardization: This is a classic problem. One system records a patient’s gender as “M,” while another uses “male.” Without a clear translation map, the systems can’t understand each other. This requires careful data mapping to get right.
-
Legacy Systems: So many hospitals and clinics rely on older, workhorse systems that were built long before modern APIs were common. Connecting to them often means building custom, sometimes brittle workarounds that take a lot of specialized expertise.
-
Security and Compliance: As you connect more systems, you create more pathways for data to travel, and more potential points of failure for security. Maintaining robust security and ensuring every connection is compliant with HIPAA is a non-negotiable, ongoing challenge that needs expert cyber compliance solutions.
Can we start an integration project without a massive upfront cost?
Yes, absolutely. The days of needing a massive capital investment just to get started are mostly behind us. Modern cloud-based platforms, often called Integration Platform as a Service (iPaaS), have shifted the model to a much more predictable subscription-based operational expense.
A good partner can also help you map out a phased implementation. You can start with the integrations that will deliver the highest impact and ROI first. That early success can then help fund the next stages of your digital roadmap, allowing you to build momentum and demonstrate value without breaking the budget.
At Bridge Global, we do more than just connect systems; we build intelligent, secure, and future-ready healthcare ecosystems. As a dedicated healthtech software development partner, our expertise ensures your integration project delivers real, measurable results for your clinicians and the patients they serve.



