A Guide to Enterprise Healthtech Platform Development
Most healthcare CTOs aren’t starting from a blank page. They’re inheriting a stack of partial solutions: an EHR that runs core clinical workflows, departmental tools that don’t share context cleanly, patient-facing apps that solve one slice of the journey, and reporting layers that still depend on manual reconciliation. Teams call it transformation, but on the ground, it often feels like controlled fragmentation.
That’s why enterprise healthtech platform development has become a board-level conversation. It isn’t another software project. It’s the operating model for how clinical, operational, and financial workflows connect. When the platform is designed well, data moves with purpose, AI has the context it needs, compliance is built into delivery, and new services can be added without rebuilding the estate every time.
The scale of this shift is hard to ignore. The healthcare enterprise software market is valued at USD 43.62 billion in 2024 and is projected to reach USD 158.63 billion by 2034 at a CAGR of 13.8%, driven by demand for integrated, cloud-based systems that improve access, security, and scalability, according to healthcare enterprise software market sizing analysis.
A practical response starts with architecture, governance, and delivery discipline. It also starts with choosing the right healthtech software development partner when internal teams need deeper healthcare engineering, AI, and compliance execution.
Introduction: The Shift from Fragmented Systems to Unified Health Ecosystems
A fragmented healthcare stack creates predictable failure points. Clinicians re-enter data. Operations teams work around missing integrations. Product leaders struggle to launch anything cross-functional because every improvement depends on exceptions, interfaces, and approvals scattered across vendors.
The problem isn’t just technical debt. It’s those disconnected systems that block enterprise decisions. You can’t standardize workflows across specialties, govern AI reliably, or support modern patient journeys if your data model, identity model, and security model all live in different places.
Why unified platforms are replacing point-solution thinking
An enterprise platform gives health systems and digital health companies a shared backbone. That backbone usually includes identity, consent, interoperability, workflow orchestration, analytics, auditability, and a delivery model that supports continuous change without destabilizing regulated operations.
Three changes are pushing this shift:
-
Care delivery is cross-channel: Patients move between in-person, virtual, remote monitoring, and asynchronous interactions. Platforms need to preserve continuity across those transitions.
-
AI needs usable data foundations: A model is only as useful as the context, controls, and workflow integration around it.
-
Compliance is now architectural: Regional privacy rules, audit demands, and data-locality expectations affect platform design from day one.
Unified health ecosystems aren’t built by connecting everything to everything else. They’re built by deciding which capabilities become enterprise services and which remain local.
What a CTO should optimize for first
The first decision isn’t framework selection or cloud vendor preference. It’s whether the organization is building for system coherence or just accelerating local projects. Those are different programs.
A coherent platform strategy usually focuses on:
-
Shared data contracts: Clear rules for how clinical, operational, and financial data are exchanged and validated.
-
Workflow fit: The platform has to support how care and administration happen, not how process documents claim they happen.
-
Extensibility: New modules, AI agents, and partner solutions should plug in without destabilizing core workflows.
The approach to many programs determines whether they become durable or expensive. If the organization treats the platform as a product with a long operating life, decisions improve. If it treats it as a one-time implementation, rework starts almost immediately.
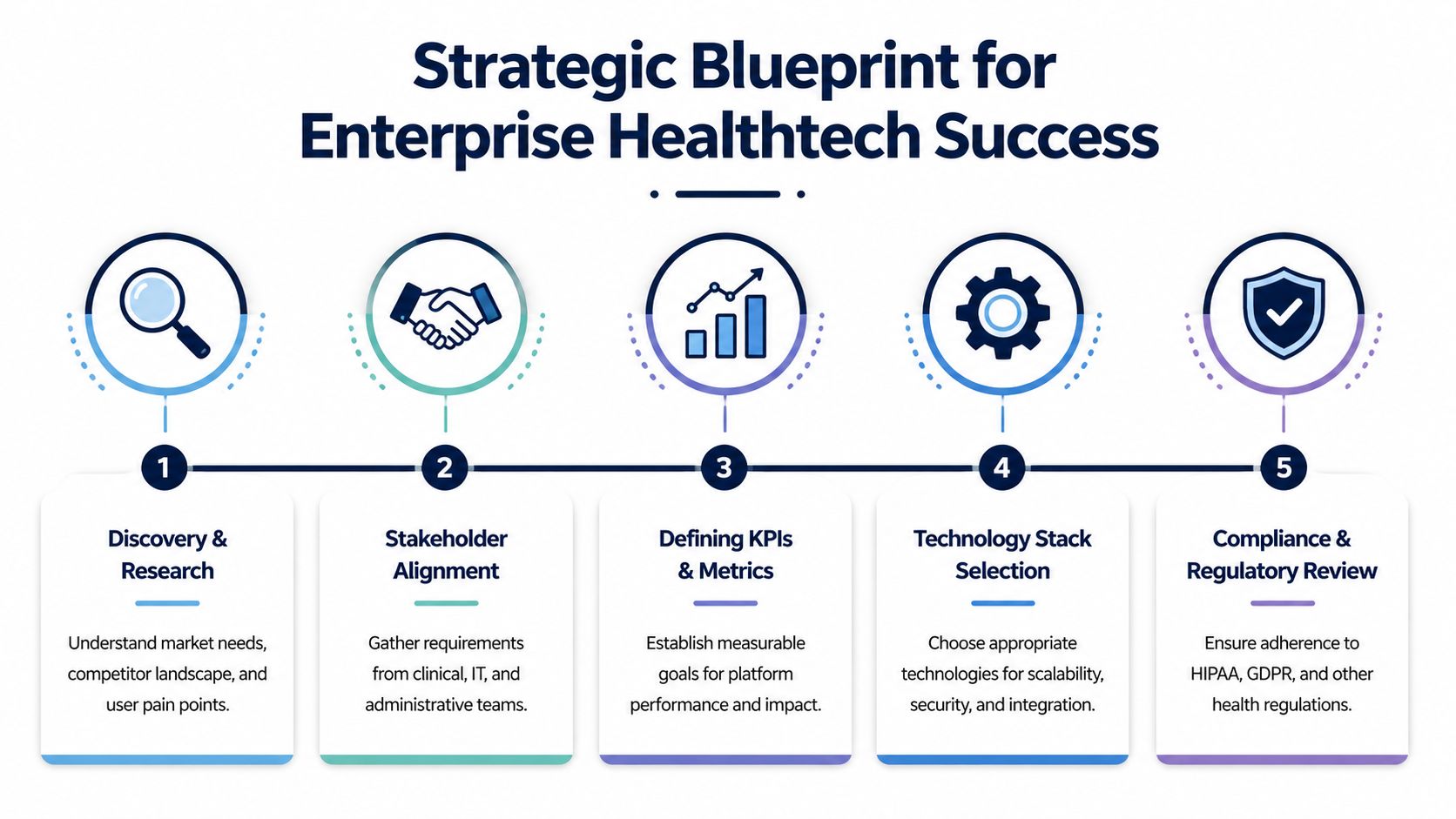
Phase 1: The Strategic Blueprint for Platform Success
Monday morning. The CTO wants a unified patient platform in 12 months. The CMIO wants fewer clicks for clinicians. Revenue cycle wants cleaner intake and fewer denials. Compliance wants defensible consent, access controls, and audit history. If Phase 1 starts as a requirements-gathering exercise, the program usually heads toward expensive rework. The primary objective is to define the platform as a business capability with clear operating rules, not a collection of features.
Research on digital health platforms points to eight recurring capability areas: human-centered design, operational workflow, clinical content management, communication channels, reporting and analytics, standards-based integration, security and data management, and scalability, as outlined in this digital health capability framework. The mistake is treating them as separate workstreams. Enterprise healthtech programs succeed when those capabilities are planned as one system, with strategy, AI readiness, compliance, and delivery capacity tied together from the start.
Start with workflow truth
Interviews alone do not produce a reliable blueprint. Clinicians describe intended care paths. Operations managers describe workarounds that keep the day moving. IT describes the current application estate and integration pain. Compliance describes policy boundaries. Each view is valid, but the platform should be shaped by observed behavior across the care journey.
A stronger discovery pattern usually includes four moves:
-
Observe live workflow paths across access, scheduling, documentation, orders, referrals, billing, messaging, and follow-up.
-
Document exceptions and handoffs such as missing prior authorization, incomplete demographics, credentialing gaps, or care-team reassignment.
-
Separate enterprise services from local preferences so that every department does not turn its habits into platform architecture.
-
Test proposed workflows against policy and scale before they enter the roadmap.
Exception mapping matters more than many teams expect. In healthcare, trust is won or lost in edge cases. A referral without complete coverage data, a telehealth visit that changes to in-person, a consent update after intake, or an expired provider credential can break the workflow and expose compliance gaps. Teams that need provider onboarding context can find credentialing insights on WeekdayDoc.
Set one primary outcome, then enforce guardrails
A platform program needs a single top-level outcome. Reduce clinician documentation time. Improve patient access across channels. Raise service-line coordination. Improve revenue-cycle accuracy. Pick one. Without that choice, the roadmap turns into a negotiation between departments with incompatible priorities.
Guardrails keep that North Star from creating blind spots:
-
Clinical guardrail: The workflow should reduce ambiguity, duplicate entry, or handoff risk for care teams.
-
Operational guardrail: The platform should remove manual coordination steps, not shift them to another team.
-
Compliance guardrail: The organization should be able to explain data movement, access decisions, and consent state in plain terms.
-
Commercial guardrail: The operating model should support reimbursement, utilization control, and partner obligations.
-
Technical guardrail: New modules should fit the platform without forcing identity, data, or integration redesign.
I have seen programs approve features that solved a local pain point but created downstream problems in role design, consent handling, or audit review. Those features looked productive in demos and expensive in production.
Practical rule: If a proposed feature cannot be mapped to workflow ownership, policy ownership, and runtime ownership, it is not ready for delivery.
Treat equity as a platform design decision
Equity work belongs in Phase 1 because access assumptions get embedded early. Channel mix, language support, device expectations, care routing, and escalation models all affect who can use the platform successfully. If those choices are deferred, the platform will favor the patients and providers who already fit the default workflow.
That changes design choices quickly.
| Decision area | Weak approach | Better enterprise approach |
|---|---|---|
| Access channels | One digital path for all users | Supported paths across app, portal, contact center, and assisted service workflows |
| Specialist access | Local scheduling logic only | Network-aware routing with escalation and capacity rules |
| Content design | Generic patient messaging | Context-aware content by language, need, literacy level, and care setting |
This is not only a patient experience issue. It affects throughput, no-show recovery, service-line utilization, and reporting quality.
Match ambition to delivery capacity
Many organizations can describe a five-year target state. Fewer can support the release cadence, integration testing discipline, governance reviews, training model, and uptime expectations needed to reach it. Platform strategy has to reflect operating reality.
That is why early planning should test three things at the same time: what the business needs, what the architecture can support, and what the organization can govern. A phased plan grounded in actual delivery capacity produces better results than an oversized roadmap with weak execution control. For teams aligning cloud operating decisions with platform goals, this healthcare cloud transformation roadmap is a useful reference. For organizations shaping AI-enabled operating models, an AI transformation framework can help sequence platform capabilities, data readiness, and governance work before teams commit to building.
The same discipline applies to engineering choices. For new products and legacy modernization programs, custom software development should be reserved for workflows that create real strategic value. Commodity functions often belong in configured products or partner services. The blueprint should make that distinction early, because custom code carries a long maintenance tail in regulated environments.
Phase 2: Architecting a Compliant and Future-Ready Foundation
Architecture decisions get framed as technology choices, but in healthcare, they’re governance choices first. You’re deciding where sensitive data lives, how systems fail, who can change what, and whether regional constraints can be respected without crippling delivery speed.

Compliance-by-design changes the architecture shape
Teams that bolt compliance on later usually discover they’ve created hidden coupling. PHI flows through the wrong services. Logging is inconsistent. Role models don’t map to real clinical access patterns. Audit trails can’t explain workflow decisions clearly.
A stronger foundation starts with a few hard rules:
-
Data classification first: Separate PHI, operational metadata, analytics data, and derived AI artifacts early.
-
Identity architecture before feature architecture: SSO, role-based access, delegated access, and service-to-service trust need a coherent plan.
-
Auditability as a platform service: Logging, traceability, and policy enforcement shouldn’t be left to each feature team.
For many organizations, the right answer is a cloud-first foundation with selective edge or hybrid controls where latency, sovereignty, or facility-level operations demand it. If you’re evaluating migration patterns, our guide to healthcare cloud transformation outlines the practical sequence teams usually need.
Monolith versus microservices in healthcare
This choice gets oversimplified. Microservices aren’t automatically mature, and monoliths aren’t automatically obsolete. In healthcare, the critical question is where you need independent scaling, independent release cycles, and strict isolation boundaries.
A useful comparison looks like this:
| Architecture style | Usually works best when | Main risk |
|---|---|---|
| Modular monolith | The domain is still stabilizing and teams need shared transaction boundaries | Overgrowth into a tightly coupled core |
| Microservices | Multiple teams need independent releases across distinct domains like scheduling, communications, consent, and analytics | Operational overhead and fragmented observability |
For many mid-market enterprises, a modular monolith with clear domain boundaries is the better first move. It preserves delivery speed while avoiding premature service sprawl. Then, specific domains can be extracted when scale, performance, or organizational structure justifies it.
Integration architecture is where many foundations crack
Healthcare systems rarely fail because engineers can’t write APIs. They fail because vendor processes, data semantics, and operational assumptions don’t line up. Credentialing is a good example. It looks administrative until it blocks onboarding flows, provider matching, scheduling, and payer interactions. Leaders who need a primer on those dependencies can find credentialing insights on WeekdayDoc.
Build the integration layer like a product:
-
Canonical data model: Don’t let every upstream system dictate your downstream logic.
-
Normalization services: Device data, lab feeds, and EHR variations need transformation and validation before they touch business workflows.
-
Failure handling: Retries, dead-letter queues, reconciliation jobs, and operator dashboards are not optional in clinical environments.
If your architecture diagram has clean arrows but no visible reconciliation path, the real system hasn’t been designed yet.
Security posture has to support delivery, not block it
Security teams often inherit the reputation of saying no because engineering invites them in too late. In healthy platform programs, security architects help define deployment pipelines, secrets handling, environment segregation, evidence collection, and release gates from the start.
That’s the difference between periodic compliance theater and operational trust. It’s also where dedicated cyber compliance solutions matter. The point isn’t a checklist. It’s a repeatable security model that supports feature delivery, partner integrations, audits, and incident response without forcing the team to reinvent controls every sprint.
Phase 3: Weaving Intelligence with AI and Data Engineering
A common failure pattern shows up after the platform foundation is in place. The team has clean APIs, controlled environments, and a backlog full of AI ideas. Then the first pilot hits real workflow data. Timestamps conflict, labels are incomplete, and nobody can explain why one recommendation was generated and another was suppressed. At that point, AI stops being an innovation project and becomes an architecture problem.
Healthcare organizations are under pressure to reduce documentation burden, route work faster, and spot risk earlier. AI can help with all three. The mistake is treating models as a layer you add later, after strategy, compliance, and data design are already set. In enterprise healthtech platform development, intelligence has to be designed as part of the operating model from the start. Otherwise, teams end up rebuilding data contracts, approval flows, and audit controls after pilots are already in production.
The market is moving quickly. Analysts at Mordor Intelligence project strong growth in enterprise healthcare AI adoption in this enterprise healthcare AI market analysis. The more important point for CTOs is practical. Buyers are no longer asking whether AI belongs in the platform. They are asking where it creates measurable operational value without creating new compliance risk.

Pick AI use cases based on workflow pressure, not model novelty
Start where work is already slowing the organization down. A referral queue with inconsistent prioritization. Clinicians are losing hours to note cleanup. Support teams answering the same status questions across portals, messages, and calls. Those are good candidates because the baseline pain is visible, the outcome can be measured, and the human oversight path is clear.
In enterprise programs, the use cases that hold up best usually fall into four groups:
-
Documentation assistance: Ambient note generation, summarization, coding support, and order drafting.
-
Operational triage: Intake classification, referral routing, exception flagging, and queue prioritization.
-
Risk visibility: Patient stratification, care-gap detection, and utilization forecasting.
-
Service support: Conversational guidance for scheduling, status checks, benefits questions, and patient navigation.
A narrower example is conversational support. Teams exploring intake or support automation can review this guide to an AI chatbot in a healthcare platform strategy. The value is rarely the bot itself. The value comes from how well it connects to identity, workflow context, escalation rules, and the systems that resolve the request.
Data engineering decides whether AI is trustworthy
Most healthcare AI failures start much earlier than model selection. They start with weak event design, inconsistent terminology, poor provenance, and missing operational context. If the platform cannot explain where a data point came from, when it changed, and which policy applies to it, the model output will be hard to trust and harder to defend in an audit.
A usable AI layer usually requires four data disciplines:
-
Traceable ingestion. Each record needs a source trail, transformation history, and version context.
-
Normalization against shared schemas. Clinical, claims, device, and engagement data cannot arrive in whatever shape the source system prefers.
-
Policy-aware processing. Retention, masking, access scope, and model eligibility rules need to be applied before data reaches inference or training pipelines.
-
Output instrumentation. Recommendations, summaries, and classifications need confidence signals, human review points, override paths, and logging.
This is the trade-off many teams underestimate. Fast pilots are attractive, but in healthcare, speed without data discipline usually creates expensive rework. The first version may demo well. The second version, the one that has to survive compliance review and cross-functional adoption, is where weak foundations show up.
Governance has to cover the full decision path
Enterprise buyers do not approve of AI because a model performs well in isolation. They approve it when the platform can control how the model is used, who can change it, how outputs are reviewed, and what happens when performance drifts. That means clear release approval for prompts and models, rollback procedures, audit logs for AI-assisted actions, and evaluation tied to actual workflow outcomes.
It also means drawing a hard line between assistive and autonomous behavior. Summarization with clinician review has one risk profile. Routing a referral automatically, based on inferred urgency, has another. Good architecture makes that distinction explicit in permissions, UX, logging, and operational policy.
Many organizations bring in external AI development services at this stage because internal teams know the clinical problem but need help building evaluation frameworks, MLOps controls, and production-grade data pipelines. Bridge Global’s role in these programs is usually practical rather than theoretical: connect AI delivery to the platform architecture, compliance model, and release process so intelligence becomes a managed capability instead of a collection of disconnected pilots.
Some lessons transfer from outside healthcare. Benely’s perspective on the future of HR with AI is useful for one reason in particular. It shows how AI changes approvals, roles, and daily work patterns long before the technology story is fully settled.
AI should enter healthcare through governed workflows with accountable owners, defined review paths, and measurable operational outcomes.
Phase 4: Ensuring Seamless Adoption and Interoperability
A platform can be clinically sound, secure, and technically elegant, yet still fail because users don’t trust the handoffs. Adoption usually breaks at the seams. A clinician opens the screen and doesn’t see the right context. A coordinator waits for data that arrived in the sandbox but not in production. A patient completes intake, but the information lands in a queue nobody owns.
That’s why interoperability and usability have to be designed together.

The EHR bottleneck is rarely just an API problem
In enterprise healthtech platform development, EHR integration is the most common source of project delays, driven not only by engineering complexity but by vendor credentialing, sandbox-to-production differences, and FHIR implementation variation. Teams that plan realistically allocate a 30 to 40 percent timeline buffer for integration phases compared with sandbox estimates, based on this healthcare software development guide.
That buffer sounds conservative until you’ve lived through a rollout where test data looked clean, production permissions arrived late, and one workflow required a different auth path than expected.
What actually reduces integration pain
A reliable pattern looks less glamorous than most architecture decks:
-
Contract-first integration design: Define payloads, error states, version handling, and ownership before building UI dependencies.
-
Environment parity checks: Treat sandbox and production as different systems until proven otherwise.
-
Operational acceptance testing: Test what users need to complete in practice, not just whether the API returns a valid response.
If you’re planning a modernization program with heavy interoperability requirements, our overview of EHR integration services covers the delivery mechanics in more depth.
Production readiness in healthcare means the workflow works with real credentials, real latency, real exceptions, and real accountability.
Adoption depends on workflow respect
Healthcare users abandon tools that ask them to leave their working context. Clinicians won’t tolerate extra navigation for basic actions. Front-desk teams won’t trust a platform that hides eligibility or scheduling ambiguity. Patients won’t persist with portals that assume perfect literacy, device access, or attention.
A few design choices consistently help:
| User group | Common mistake | Better design choice |
|---|---|---|
| Clinicians | Forcing context switches across modules | Embed actions in the existing encounter or task flow |
| Coordinators | Hiding status across handoffs | Show queue state, ownership, and next action clearly |
| Patients | Assuming one digital channel fits all | Offer assisted, asynchronous, and mobile-friendly paths |
QA in healthcare has to reflect clinical consequence
Generic regression testing isn’t enough. Teams need scenario-based validation that reflects downtime risk, delayed data arrival, duplicate records, stale alerts, and role-specific visibility rules. The test plan should include a clinical safety review where the workflow touches care decisions, documentation, or time-sensitive coordination.
The strongest teams make QA cross-functional. Product, engineering, compliance, clinical operations, and support all review the same critical-path scenarios. That catches the defects that unit tests miss: misleading labels, wrong escalation routing, hidden dependencies on vendor response times, and edge-case failures that only appear in realistic care transitions.
Phase 5: Launch Governance and Scaling for Long-Term Value
Go-live isn’t the finish line. It’s the point where platform quality becomes visible to the organization every day. The question changes from “can we ship it?” to “can we operate it without drift, confusion, and governance debt?”
That’s where many enterprise programs lose momentum. The build team hands over a working platform, but nobody owns decision rights for workflow changes, data definitions, AI updates, or third-party additions.
Choose a rollout model that fits clinical reality
A big-bang launch can work when the workflow is narrow, the users are tightly coordinated, and dependencies are contained. Most enterprise healthcare environments don’t look like that. They have multiple service lines, vendor touchpoints, training constraints, and operational variations that punish simultaneous change.
A phased rollout usually works better when the platform affects more than one domain. Good sequencing often starts with one bounded workflow, one controlled user cohort, and one clear operational owner. Then the team expands based on observed friction, not just planned milestones.
A rollout checklist should include:
-
Operational ownership: Name who owns triage, incident review, content changes, and release approvals.
-
Data stewardship: Define who can change mappings, business rules, and downstream reporting logic.
-
Clinical review: Establish who signs off on workflow changes that affect care delivery or documentation.
-
Vendor coordination: Track which external dependencies can delay releases or degrade service.
Governance should be lightweight, but real
Governance fails when it’s either absent or ceremonial. The practical middle ground is a small decision forum with authority across product, engineering, security, clinical operations, and analytics. It should review platform changes based on risk, not bureaucracy.
That forum usually owns:
-
Release policy
-
Exception handling standards
-
Access model changes
-
Third-party integration approvals
-
AI oversight and retraining decisions
-
Service level expectations and incident patterns
A stable operating model often needs a persistent, dedicated development team, not just project-based staffing. Healthcare platforms evolve continuously. They need engineers and product people who remember why decisions were made, not just how the code works.
Build for modular expansion, not repeated reinvention
Leading health systems are moving toward modular, interoperable platforms that support a plug-and-play ecosystem for third-party solutions, helping them avoid expensive integration-by-acquisition approaches and make better use of fragmented data and provider availability, as discussed in Deloitte’s transformed health care ecosystems analysis.
That idea matters because scale rarely comes from rebuilding the core. It comes from exposing stable platform services so new modules can attach cleanly. Scheduling, communications, identity, consent, analytics, and workflow orchestration should be reusable capabilities, not reimplemented in every new initiative.
That’s where mature product engineering services make a difference. They support the move from project delivery to platform operations. Real-world client cases are often most useful here, not as marketing proof, but as evidence that the partner understands post-launch support, controlled expansion, and cross-functional ownership.
Conclusion: Building Your Future Healthtech Ecosystem
A CTO usually sees the platform problem late. One team has shipped a patient app, another has modernized scheduling, a third is piloting AI for documentation, and compliance is still being handled as a review step. The result is predictable. Integration work grows, audit gaps appear, and every new release costs more than the one before it.
Enterprise healthtech platform development succeeds when the business model, operating model, architecture, data design, and compliance controls are built as one program. That is the difference between a collection of digital health projects and an enterprise platform that can support clinical growth, payer demands, AI adoption, and new service lines without repeated rework.
The durable approach starts earlier than many organizations expect. It starts by defining which workflows matter, which systems remain authoritative, where AI is allowed to act, and which controls have to be enforced in code rather than policy documents. Those choices shape everything that follows, from integration patterns to release governance.
I have seen strong teams lose time by treating HIPAA, FHIR, AI governance, and product delivery as separate tracks. In practice, they are tightly coupled. If consent, identity, auditability, and data quality are not designed into the platform from day one, scaling later becomes slower, more expensive, and harder to govern.
That is why the right delivery partner is not just filling engineering capacity. The job is to help structure decisions across clinical context, platform architecture, compliance boundaries, and long-term ownership. Teams such as Bridge Global are often brought in for that reason. They help organizations build a healthtech ecosystem that can keep changing without losing control.
Frequently Asked Questions
How should a CTO deal with legacy systems that can’t be replaced quickly?
Treat legacy systems as constraints to be managed, not excuses to delay platform work. Start by identifying which systems are systems of record, which are workflow tools, and which are only being kept alive because nobody has extracted their hidden logic yet.
Then create an integration boundary around them. Don’t let each new product team connect to legacy tools in its own way. Put a controlled interoperability layer in front of those systems, normalize the data, and expose stable contracts to the rest of the platform.
What’s the right first release for an enterprise platform?
Pick a workflow that is painful, visible, and bounded. It should matter enough to justify change, but not be so broad that every unresolved dependency lands in the same release. Intake orchestration, referral coordination, documentation support, or a cross-channel patient communication workflow are common candidates.
A good first release proves three things. The architecture holds. Users trust it. Governance can support change without slowing the team down.
How do you measure platform ROI without oversimplifying it?
Don’t reduce ROI to one financial metric too early. In healthcare, platform value often appears first as reduced manual coordination, faster handoffs, clearer auditability, better data quality, and fewer operational workarounds.
Track a mix of signals:
-
Workflow efficiency: Time spent on manual steps, queue handling, and duplicate entry
-
Adoption quality: Active usage in intended workflows, not just logins
-
Reliability: Incident patterns, failed handoffs, and recovery time
-
Governance health: How quickly policy, content, or integration changes can be made safely
When should an organization build in-house versus partner?
Build in-house when the capability is core, the internal team has a healthcare delivery context, and there’s capacity for long-term ownership. Partner when the platform needs specialized interoperability, regulated cloud architecture, AI engineering, or delivery acceleration that the current team can’t absorb without risking execution.
The best partner model usually isn’t full outsourcing. It’s a blended setup where internal leaders keep strategic control and an external team adds depth in the places that are hardest to staff quickly.
What’s the biggest mistake in enterprise healthtech platform development?
Treating discovery, engineering, compliance, and rollout as separate phases with separate owners. That creates rework almost immediately. Platform decisions in healthcare are cross-functional by nature. If those functions only meet at approval gates, the platform will reflect organizational silos instead of solving them.
If your organization is planning a new platform, modernizing a legacy estate, or evaluating how to embed AI into compliant healthcare workflows, Bridge Global can support the work with healthcare-focused engineering, AI-led product strategy, cloud modernization, and long-term delivery teams.



