A Guide to AI Integration in Healthtech Platforms for 2026
For a long time, healthcare felt like the last frontier for new technology. That’s changing, and fast. We’re well past the point of AI being a theoretical concept; it’s happening on the ground, in hospitals and clinics, right now. In fact, 22% of healthcare organizations are already using AI tools built for their specific needs.
This isn't just about chasing the latest tech trend. It's a fundamental shift driven by real-world results in patient care and clinical efficiency.
The AI Shift in Healthcare Is Real and Accelerating
If you think healthcare is slow on the uptake, you might want to look again. The industry is now embracing enterprise AI at more than double the pace of the broader economy. It's a remarkable turnaround.
We're seeing health systems leading the charge with a 27% adoption rate, followed by outpatient providers at 18% and payers at 14%. Why the sudden momentum? It comes down to data. Healthcare has always been data-rich, but AI finally gives us the power to make sense of it all, accelerating everything from drug discovery to day-to-day diagnostics.
From the Lab to the Bedside
AI has officially left the research papers and entered clinical practice. These aren't just vague algorithms; they are sophisticated, practical tools that are already making a difference. We see it in niche applications that are rapidly becoming mainstream, like the innovations in AI-powered fertility tracking. You can see some powerful examples in these Hera Fertility resources.
The core benefits we're seeing in the field are straightforward and impactful:
- Smarter Diagnostics: AI is proving exceptionally good at analyzing medical images and lab work, often catching subtle patterns that are nearly impossible for the human eye to see.
- Reclaiming Clinician Time: By automating tedious but necessary tasks like charting and billing, AI frees up doctors and nurses to do what they do best: care for patients.
- Truly Personal Medicine: AI can sift through a patient's entire history and genetic makeup to help predict their response to therapies, paving the way for truly individualized treatment plans.
- Predictive Health Management: On a larger scale, AI models help hospitals manage resources, predict patient surges, and even get ahead of potential disease outbreaks.

This isn't just about bolting on a new feature. It's about fundamentally rethinking how healthcare works. AI gives us a credible path toward a system that is more proactive, precise, and patient-focused.
How to Approach Your AI Integration
Getting AI right is about more than just having the best algorithm. From my experience, the biggest hurdles are navigating the maze of data requirements, airtight security and compliance, and ensuring the final tool actually fits into a clinician's workflow without causing more headaches.
This is where having a partner who's been there before becomes invaluable. Working with a dedicated healthtech software development partner can make all the difference. An experienced team helps you build a practical roadmap—from the initial idea to a full-scale deployment—so your AI initiatives don't just look good on paper but deliver real, measurable improvements for your patients and your bottom line.
Building Your Foundation with Strategy and Data Readiness
Let's be blunt: most AI in healthtech doesn't fail because of a bad algorithm. It fails because of a bad start. Too many teams get excited about the tech and dive straight into coding, completely skipping the two things that matter most: a solid strategy and clean, ready-to-use data.
It all begins with pinpointing exactly where AI can make a real difference. Forget the buzzwords for a moment. Think about the nagging, everyday problems your clinicians and administrators face. Could you predict patient no-shows to optimize scheduling? What if you could automatically summarize dense clinical notes to save doctors hours each week? Or identify at-risk patient populations right from your EHR data?
This is where a focused AI Discovery Workshop becomes your most valuable first move. Bringing your clinical, tech, and business leaders into one room helps you zero in on use cases that actually align with your organization's goals and have a clear path to delivering value. This strategic alignment is a core part of our AI transformation framework.
Getting Your Data House in Order
Once you’ve picked a high-impact problem to solve, your focus has to pivot entirely to the data. I’ve seen this trip up more healthtech initiatives than anything else. An AI model is a mirror of the data it’s fed, and in healthcare, that data is notoriously complex.
Data readiness isn't about volume. It’s about having the right data, structured correctly, and accessible in a way that’s both secure and efficient. This is often the most grueling part of the journey. To get a better handle on where you stand, as we explored in our guide, you can assess your organization's AI readiness.

Before you write a single line of code, you have to get brutally honest about your data infrastructure—its quality, how it talks to other systems, and how it’s protected.
Never underestimate the sheer effort it takes to clean and structure healthcare data. Information from EHRs, wearables, and claims systems is often trapped in silos, wildly inconsistent, and just plain messy. Committing resources to wrangle this data isn't optional; it's the only way to build reliable AI.
To help you get organized, we've created a simple framework to evaluate potential AI projects. This matrix helps you weigh the clinical benefits against the technical lift, so you can prioritize what to tackle first.
AI Use Case Prioritization Matrix for Healthtech
| Use Case Category | Example Application | Clinical Impact (Low/Med/High) | Technical Feasibility (Low/Med/High) | Implementation Priority |
|---|---|---|---|---|
| Operational Efficiency | AI-driven patient scheduling and no-show prediction | Medium | High | High |
| Clinical Decision Support | Sepsis risk prediction from real-time EHR data | High | Medium | High |
| Medical Imaging | Automated detection of nodules in chest X-rays | High | Medium | Medium |
| Administrative Automation | NLP for summarizing physician's notes for billing | Medium | High | High |
| Patient Monitoring | Wearable data analysis for chronic disease management | Medium | Medium | Medium |
| Drug Discovery | Identifying novel drug targets from genomic data | High | Low | Low |
Focusing on the high-impact, high-feasibility use cases first allows you to build momentum and demonstrate value quickly, which is key for getting long-term buy-in for more ambitious projects.
Your Data Infrastructure and Pipeline Checklist
To build a data pipeline that can actually support a production-grade AI model, you need to check a few boxes. Think of this as your pre-flight checklist.
- Data Quality and Integrity: Is the data accurate and complete? More importantly, do you have automated ways to spot and fix errors before they pollute your model?
- Interoperability: Can you pull data from your EHR, LIS, and PACS systems without a massive headache? Standards like FHIR and HL7 are your best friends here.
- Data Accessibility: Can your data science team get the data they need securely and without waiting weeks? Delays here will kill your project's momentum.
- Structure and Formatting: Is your data neatly structured, or is it a mountain of unstructured clinical notes? If it's the latter, you'll need a solid plan for Natural Language Processing (NLP), which adds another layer of complexity.
- Security and Governance: Do you have iron-clad security protocols for handling Protected Health Information (PHI)? This means robust encryption, strict access controls, and a clear data governance policy that everyone understands.
Getting these fundamentals right is what separates a successful AI integration from an expensive, failed experiment. Investing heavily in strategy and data prep at the beginning isn't just a best practice—it's the only way to ensure your AI solution will perform accurately, safely, and effectively in a real-world clinical setting.
Navigating Healthtech Compliance and AI Security
In healthcare, trust isn't just a buzzword; it's the currency of every interaction. When you’re building AI tools that touch sensitive patient data, that trust is on the line. The second your platform interacts with Protected Health Information (PHI), you're not just in the tech business anymore—you're in the trust business, operating in a world governed by strict regulations like HIPAA and GDPR.
This is a world where security can't be a bolt-on feature. It has to be the bedrock. A data breach doesn't just tarnish your brand; it can bring crippling fines and legal battles, shattering the confidence of the very patients and doctors you aim to serve.
Embedding Compliance from Day One
The only way to build a successful and responsible AI-powered healthtech platform is with a "secure by design" mindset. Honestly, it's not even a choice. This work starts long before a single algorithm is deployed.
Take data de-identification, for instance. This isn't just a technical step; it's a foundational ethical and legal requirement. We meticulously strip out personal identifiers from the datasets used to train our AI models. The goal is simple: PHI should never, ever be exposed unless absolutely necessary for a specific, permitted function.
Then you have to think about where this data actually lives. Moving health data to the cloud is standard practice, but it demands an almost obsessive focus on security.
- End-to-End Encryption: Your data must be locked down tight, both when it's sitting on a server (at rest) and when it's moving across the network (in transit). No exceptions.
- Strict Access Controls: We live by the principle of least privilege. If a user doesn't absolutely need to see a piece of data to do their job, they don't get access. It’s that straightforward.
- Comprehensive Audit Trails: You need an unchangeable record of every single touchpoint with the data. Who accessed it? When? What did they do? This creates a crystal-clear trail for compliance checks and security reviews.
Trying to tack on security and compliance measures after the fact is a recipe for disaster. It’s like a surgeon deciding where to make the incision after they’ve already closed the patient up. It's ineffective, costly, and frankly, negligent.
Conducting Rigorous Risk Assessments
Before any AI tool sees the light of day, it needs to go through a comprehensive risk assessment. We’re talking about a top-to-bottom analysis to proactively hunt down vulnerabilities, whether they're in the code, your operational procedures, or even potential human errors. Every part of your system gets put under the microscope—from the initial data entry points to the APIs connecting with an EHR.
When you're handling the health data of EU citizens, you have to be fluent in the language of data processing agreements and GDPR. Understanding the nuances is non-negotiable. For a detailed guide on this specific topic, there's a great resource here: Mehr zu Dsgvo Compliance mit reruptionchat. This is the kind of homework that separates responsible innovators from reckless ones.
Back in the U.S., the landscape is dominated by HIPAA, and building compliant software requires its own specialized playbook. As we've detailed in our guide on HIPAA compliant software development, there's a proven methodology to meet these stringent requirements.
Ultimately, navigating this regulatory maze isn't a DIY project. Getting it right demands deep expertise, which is why working with a partner who specializes in cyber compliance solutions ensures your platform isn’t just innovative, but also fundamentally trustworthy and secure from its very core.
Alright, you’ve sorted out your strategy and your data is ready to go. Now comes the exciting part: turning your AI vision into a real, working tool that clinicians can actually use. This is where the technical heavy lifting happens, but it's more than just coding. It's a delicate balance between building a powerful algorithm and making sure it can be reliably deployed, monitored, and maintained in a live clinical environment.
This phase is all about moving from a promising proof-of-concept to a robust, compliant solution that seamlessly fits into healthcare workflows.
First Up: Model Selection and System Architecture
One of the first major decisions you'll face is whether to build a custom AI model from scratch or adapt a pre-trained one. This choice will ripple through your entire project, affecting your timeline, budget, and the final performance of the tool.
- Building a Custom Model: If you're tackling a completely new problem or have unique, proprietary data, building from the ground up is often the only way to get the accuracy and competitive edge you need. It’s more intensive, but the results can be tailored precisely to your use case. As we explored in our guide, choosing between custom and pre-trained healthcare machine learning models is a critical step.
- Using Pre-trained Models: For more common tasks, like identifying standard anomalies in medical images, starting with a pre-trained model can give you a massive head start. These models have already learned from vast datasets, so you're not starting from zero.
While you're figuring out the model, you also need to be thinking about the system architecture. This isn't just about servers and databases; it's about designing a scalable system with clean APIs that can plug into existing EMRs, patient portals, and other clinical software. A well-designed architecture, often delivered through expert product engineering services, means your AI feels like a natural part of the tools clinicians already know.
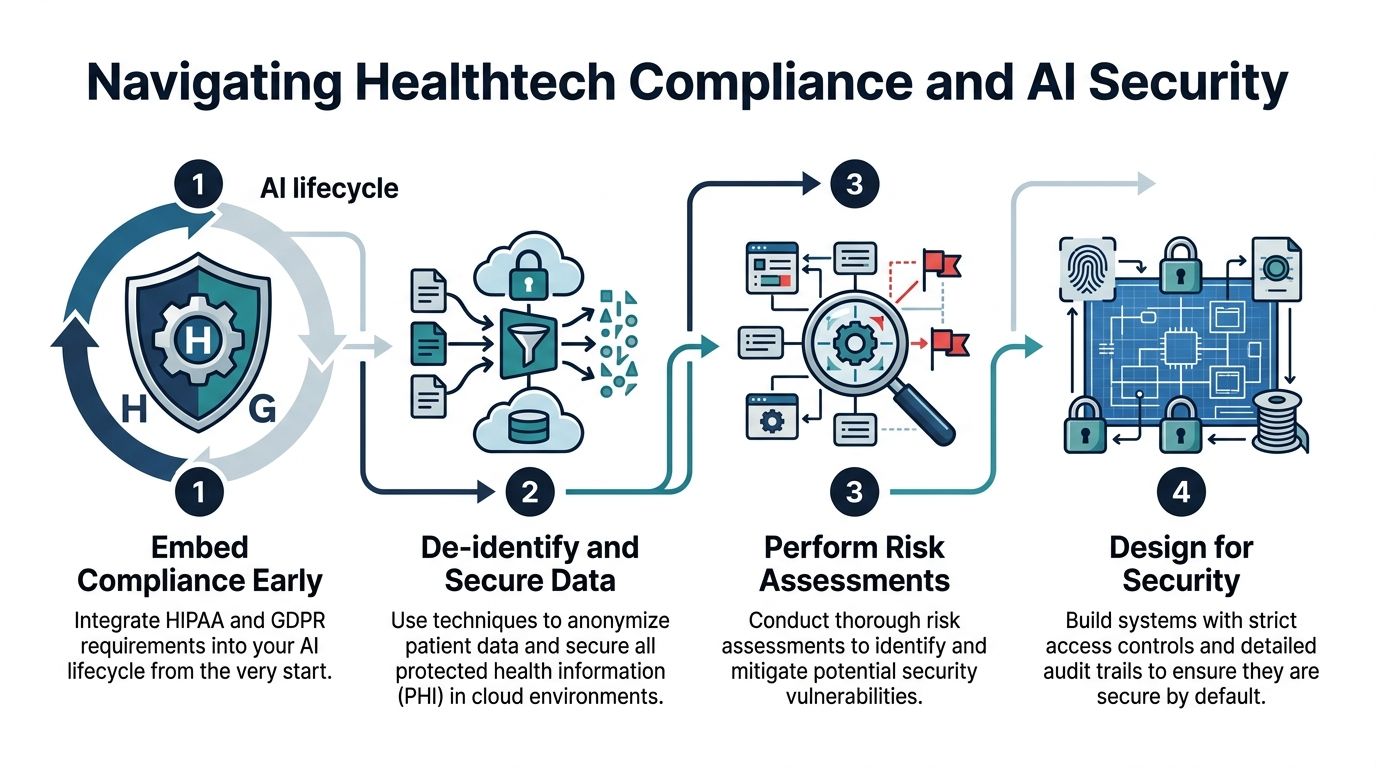
As this shows, weaving in compliance and security from the start isn't optional—it's central to building something that will actually make it into a hospital.
MLOps: The Engine That Keeps Your AI Running
An AI model isn't a "set it and forget it" piece of software. It needs constant care and feeding. That's where MLOps (Machine Learning Operations) comes in. MLOps is the set of practices for deploying, monitoring, and maintaining your models in production to make sure they stay accurate, reliable, and fair over time.
Think of MLOps as the mission control for your AI. It automates deployment, watches for performance drops, and creates a system for retraining and updating models without causing chaos in the clinic. Without a solid MLOps strategy, even the most brilliant model will eventually become useless or, worse, dangerous.
This continuous cycle is absolutely critical in healthcare. A model's performance can degrade as patient demographics change, new treatments are introduced, or even when a hospital gets a new imaging machine. MLOps helps you catch that "model drift" early. Rigorous testing is part of this, and it’s important to understand the real-world limits of AI. For example, some early tests on consumer-grade AI, like this ChatGPT's ECG reader test, highlight just how critical specialized validation is.
The Ground Reality of AI in Hospitals
AI adoption is definitely on the rise. We've seen the integration of predictive AI in EHRs at U.S. hospitals jump from 66% in 2024 to an estimated 73% in 2026. These tools are being applied to high-stakes tasks, with 93% of hospitals using them to predict inpatient risks, 88% to flag high-risk outpatients, and 67% to optimize scheduling.
But here’s the tough reality: only about 30% of AI pilots actually make it to full production. The roadblocks are predictable but challenging: security worries, poor data readiness, steep integration costs, and a very real expertise gap.
Getting through this phase successfully demands a high level of technical skill. From building out APIs to implementing a full MLOps pipeline, it's a lot to manage. This is where having a dedicated development team can make all the difference, ensuring your project moves smoothly from a promising idea to an operational tool that helps improve patient care.
Optimizing Workflows for Clinicians and Patients
I've seen brilliant AI tools gather dust on a shelf for one simple reason: they were a pain for clinicians to use. No matter how powerful the algorithm, if it disrupts a doctor's rhythm or adds another complicated step to a nurse's already packed day, it's dead on arrival. The real test for any AI integration in healthtech platforms isn't the tech—it's the human factor.
The aim is always to enhance a clinician's expertise, not to replace it. The AI should feel less like a clunky new tool and more like a trusted assistant in the exam room. This means the user interface must be so intuitive that it becomes a natural extension of the clinician's own thinking process, presenting complex insights in a way that’s immediately clear and actionable.
Designing for Trust and Clinical Adoption
For any doctor to rely on an AI's output, they have to trust it. That trust isn't built on mysterious algorithms that spit out answers with no context. It’s built on transparency and control.
From my experience, getting this right comes down to a few core principles:
- Explain the "Why": The system can't just flag a risk; it needs to show its work. This is the essence of "Explainable AI" (XAI)—presenting the data points that led to its conclusion.
- Keep the Clinician in Charge: Doctors must have the final word. The interface has to allow them to easily accept, modify, or even reject an AI's suggestion. This respects their clinical judgment and keeps them in the driver's seat.
- Make Data Visual: Nobody wants to sift through dense tables of numbers. Use clean charts, highlighted text, and simple visual cues to spotlight what matters, like an abnormal lab result or a worrying trend in vitals.
A well-designed interface is what turns a powerful algorithm into a usable clinical instrument. This is why successful custom healthcare software development always puts the end-user experience front and center. It’s the only way to drive adoption and see a real return on the technology.

Weaving AI into Existing Clinical Workflows
The smartest way to ensure a tool gets used is to avoid asking clinicians to change their habits. Instead of forcing them to learn entirely new software or processes, the best AI integrations are woven directly into the workflows they already perform hundreds of time a day.
Look at the rise of ambient scribes. These AI tools listen in the background of a patient visit (with full consent, of course) and automatically draft a structured clinical note. The physician just needs to review and sign off on it within their existing EHR system. No new software to juggle, no extra steps.
The impact is massive. Clinicians are spending less time on documentation after hours—a primary driver of burnout—and more time focused on the patient in front of them. The AI takes on the administrative load, freeing up the doctor to do what they do best: practice medicine.
This is the core idea of workflow optimization. Find a point of friction, and use AI to make it disappear without creating a new one.
Real-World Scenarios of Workflow Augmentation
The opportunities to augment workflows are everywhere. Here are a few practical examples that are already making a tangible difference in hospitals and clinics:
- Smarter Triage: In a chaotic emergency department, an AI can scan incoming EHR data to flag patients showing subtle, early signs of sepsis. The system sends an alert directly within the existing triage software, helping the team prioritize the most critical cases for immediate care.
- Patient-Facing Chatbots: An AI-driven chatbot on a hospital's website can handle routine patient questions, schedule appointments, and provide pre-visit instructions 24/7. This frees up front-desk staff to handle more complex issues and gives patients instant answers.
- Medication Safety Checks: When a doctor prescribes a new medication, an AI can instantly cross-reference it with the patient's record to flag potential adverse drug interactions. This warning pops up directly on the prescribing screen inside the EHR, acting as an immediate, critical safety net.
In all these scenarios, the AI isn't the star. It’s a quiet, efficient partner working behind the scenes, making the entire process faster, safer, and more human-centric for everyone.
Measuring What Matters: Proving Your Healthtech AI's ROI
The AI is live. The team is proud. But now the CFO is at your door asking the million-dollar question: "What's the return on this?" After all the hard work of deploying an AI solution, this is where the rubber meets the road. Proving the value of AI in a healthtech platform goes far beyond just showing that the model is accurate; you have to connect the dots between the tech and tangible improvements for patients, clinicians, and the bottom line.
This is how you justify the investment and build the momentum needed for your next big project. By tying your results directly back to the problems you set out to solve, you create a data-backed story that resonates with everyone from executives to the clinicians on the floor. It's the key to making AI a core part of your strategy, not just a one-off experiment. Think of it less as a final report and more as the first chapter in your organization's broader digital transformation consulting.
Defining Your Key Performance Indicators
To prove your AI is working, you need to measure what matters. Don't get lost in a sea of data; focus on a handful of Key Performance Indicators (KPIs) that tell the whole story. I always recommend clients track metrics across three distinct domains to get a complete picture.
Here are a few examples of what that looks like in practice:
Clinical Impact
- Fewer Diagnostic Errors: What's the percentage drop in misread medical images or misinterpreted lab results?
- Better Patient Outcomes: Are you seeing lower readmission rates? Are patients with chronic conditions showing better health markers?
- Faster Diagnoses: How much time are you shaving off between a patient’s first test and their confirmed diagnosis?
Operational Efficiency
- Higher Patient Throughput: How many more patients can you see per day now that workflows are smarter?
- Easing Clinician Burnout: Track the time physicians get back when they're not bogged down in administrative tasks like charting.
- Quicker Documentation: What’s the average time from a patient visit to a finalized, signed clinical note?
Financial Returns
- Lower Admin Costs: Calculate the direct savings from automating tedious jobs like medical coding and billing.
- Smarter Resource Use: Can you show cost reductions from AI-powered staff scheduling or better inventory management?
- New Revenue Streams: Link the AI directly to gains, like a drop in costly patient no-shows.
Building the ROI Case for Stakeholders
Once you have your KPIs, you can weave them into a compelling story about return on investment. This isn't just about spreadsheets; it’s about showing how the numbers translate into real-world value. And the good news? The data shows that many healthcare organizations are seeing a positive return, often much faster than they expected.
In fact, recent research shows that when it comes to AI in healthcare, 52% of organizations are already reporting moderate returns, with another 30% seeing high or even very high returns. It’s happening fast, too. A striking 45% of teams using generative AI saw tangible benefits in less than a year. We're seeing specific tools, like ambient clinical notes, achieve 100% adoption activity with an impressive 53% high success rate. You can dive deeper into these numbers by checking out the full research on AI in healthcare statistics.
A powerful ROI case does more than just present the numbers. It tells a story about how your technology investment solved a critical problem, directly improved patient care, and made the entire organization more efficient and financially healthy.
As we’ve seen in our own client cases, this relentless focus on measurable results is what elevates an AI project from a cool experiment to a core strategic asset. By meticulously tracking what matters, you not only prove the value of your work but also create a clear, data-driven roadmap for what comes next.
FAQs: Your Top AI Healthtech Questions Answered
When we sit down with healthcare leaders, the same crucial questions about AI integration in healthtech platforms come up time and time again. Moving into AI involves big strategic decisions, so let's tackle some of the most common concerns.
What Is the Biggest Challenge of AI Integration in Healthtech?
Almost every single time, the biggest hurdle is data readiness and security. It's the unglamorous but essential foundation. Healthcare data is notoriously messy—it's often siloed in different systems, unstructured (like doctors' notes), and, of course, protected by strict regulations like HIPAA.
If you don't get the data pipeline right from day one, a project can stall before it even truly begins. This is where having a partner with deep expertise in both AI development services and the nuances of healthcare compliance becomes invaluable. They can help you build that solid data infrastructure needed for any successful AI initiative.
Should We Build a Custom AI Model or Use an Existing One?
This is the classic "build vs. buy" debate, and the right answer really comes down to your specific goals and the uniqueness of your data.
For more generalized tasks, like identifying common patterns in certain medical images, a pre-trained model can get you up and running quickly and cost-effectively. But if your goal is to solve a very niche problem or you're sitting on a goldmine of proprietary data, building your own model is the way to go. A custom software development approach in this case can create a powerful competitive advantage that off-the-shelf solutions just can't match.
How Do We Get Clinicians to Actually Use New AI Tools?
Adoption lives and dies by one simple rule: the AI must fit into the existing clinical workflow and make a doctor's or nurse's life easier, not harder. You can't just drop a new tool on their laps and expect them to use it.
Involve your clinicians from the very beginning of the design process. Ask them what their biggest administrative headaches are or where faster insights would make a real difference.
The key to getting buy-in is building trust. This comes from an intuitive interface and explainable AI that shows clinicians why it's making a certain recommendation. We always recommend running pilot programs with a few clinical champions to prove the tool’s value and gather honest feedback.
Ultimately, the AI has to feel like a helpful assistant, not just another box to check.
How Can We Measure the ROI of Our AI Healthtech Platform?
Proving return on investment requires tracking metrics across three key areas: clinical impact (e.g., reduced diagnostic errors, better patient outcomes), operational efficiency (e.g., time saved for clinicians, faster documentation), and financial returns (e.g., lower administrative costs, reduced patient no-shows). By connecting your AI integration to these tangible KPIs, you build a powerful business case that justifies the initial investment and paves the way for future projects.
How Long Does It Take to See a Return on AI in Healthcare?
While it varies by project complexity, many organizations see returns faster than expected. Recent data shows that 45% of teams using generative AI reported tangible benefits in less than a year. The key is to start with high-impact, high-feasibility projects that can deliver quick wins and build momentum for your broader strategy for using AI for your business.



